Blog post by Andrew Quinn, Jemma Pitt, Méadhbh Brosnan, Sarah Clayton, & Kia Nobre from the Brain & Cognition lab & OxDARE team for Dementia Action Week 2021.
Some research studies into dementia are starting to use Magnetoencephalography scans (also known as MEG scans) but what is MEG? What does it measure? And what can it tell us about neurodegeneration?
What is MEG?
The brain uses electricity as a mechanism for communication between neurons (brain cells). Electrical activity in the neuron creates a magnetic field which can be measured at a distance. Although the magnetic field created by a single neuron is too small to detect from afar when many thousands of neurons synchronise (are active at the same time), their magnetic fields combine and become large enough to be detected just outside of the head. Using MEG we capture these magnetic fields. When neuronal communication occurs, it is immediately evident in the magnetic fields measured by MEG. This means that MEG can measure a signature of how the neurons are operating in real-time1.

What is it like to have a MEG scan?
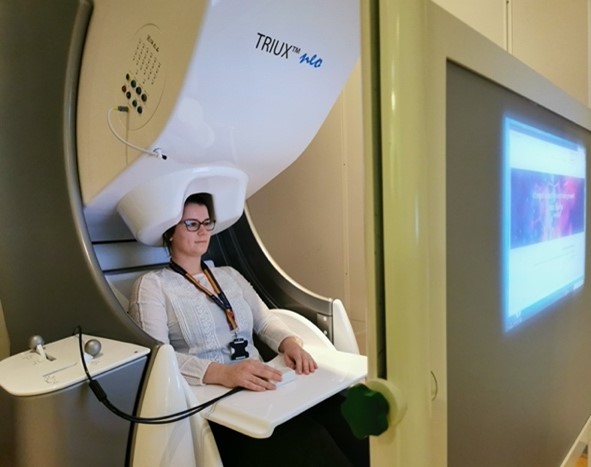
A person having a MEG scan sits upright in a chair and is raised into the scanner. This contains around 300 hidden sensors which are positioned all around the head. During a recording, the sensors can take up to one thousand measurements every second. These sensors simply ‘listen’ to naturally occurring activity in the brain and record any changes in its magnetic field over time. These magnetic fields often rise and fall rhythmically – most often between 3 and 60 times per second. What does this mean? One hypothesis is that neurons are rhythmically coordinating the sending and receiving of information to each other, to make sure they are efficiently communicating. If this synchronization is lost, then communication can become noisy or stop altogether.
What are you looking for in dementia?
MEG recordings typically feature a pattern of rhythmic activity known as the ‘alpha oscillation’. This is a fluctuation in neuronal activity in the back of the brain (known as occipital cortex) which repeats around 10 times per second. This rhythm was first described by Hans Berger in 1924 and is one of the largest signals we can record using MEG2. Research has shown that the frequency of the alpha signal appears to slow down during healthy aging3. Critically, researchers at Oxford Centre for Human Brain Activity and collaborators in Cambridge and Madrid have shown that this slowing is accelerated during early stages of Mild Cognitive Impairment and Alzheimer’s Disease (AD)4. A healthy person might show 10 cycles of the alpha signal per second but a patient with AD may only have 8 or 9 cycles in the same timespan. As the MEG signal reflects communication between neurons, these findings indicate that neurons in the brain are synchronizing less frequently in people with neurodegeneration.
This careful co-ordination between neurons might be affected in the very early stages of neurodegeneration, before widespread cell-death or severe cognitive deficits (such as problems with memory) appear. It is important to measure the very earliest changes in degeneration as this is likely to be the period when treatments or interventions are most effective, however the earliest changes are also the most subtle. The sensitive measurements coming from MEG have the potential to identify and track at precisely what point neuronal communication is just starting to become less efficient, and how this influences the severity of the subsequent progression of dementia.
What do we know already?
Most previous research into studies into MEG in neurodegeration have recruited participants from different stages of disease and made a single recording from each at one time point (this is known as a ‘cross-sectional’ design). Whilst this is effective at finding differences between large groups, it doesn’t tell us much about changes within an individual. The next generation of research using MEG in dementia are now making multiple recordings from participants over the span of one or two years (known as a ‘repeated measures’ design). These repeated recordings allow us to track any change in the activity of neurons in individual people over time. These changes can then be compared to a wide range of clinical, cognitive and lifestyle measures to see which changes in brain function are most strongly associated with progressive neurodegeneration. It is hoped that this will lead to a set of reliable and personal measures of brain function which can be used to track degeneration through the critical early stages of disease.
How can I get involved?
MEG recording is carried out in a wide range of cognitive and clinical studies at the Oxford Centre for Human Brain Activity. If you are interested in hearing more about our dementia research studies at Oxford, please contact the team on brainhealthresearch@psych.ox.ac.uk. If you experience memory difficulties and are interested in taking part in research, repeated measures MEG scans are carried out in the Deep and Frequent Phenotyping (DFP; https://www.dementiasplatform.uk/our-impact/case-studies/experimental-medicine-studies/deep-and-frequent-phenotyping-study) and New Therapeutics in Alzheimer’s Disease (NTAD; https://www.dementiasplatform.uk/our-impact/case-studies/study-into-early-alzheimers-disease-treatments) studies.
References
- https://en.wikipedia.org/wiki/Magnetoencephalography
- https://en.wikipedia.org/wiki/Alpha_wave
- Sahoo, B., Pathak, A., Deco, G., Banerjee, A., & Roy, D. (2020). Lifespan associated global patterns of coherent neural communication. NeuroImage, 216, 116824. https://doi.org/10.1016/j.neuroimage.2020.116824
- Hughes, L. E., Henson, R. N., Pereda, E., Bruña, R., López‐Sanz, D., Quinn, A. J., Woolrich, M. W., Nobre, A. C., Rowe, J. B., & Maestú, F. (2019). Biomagnetic biomarkers for dementia: A pilot multicentre study with a recommended methodological framework for magnetoencephalography. Alzheimer’s & Dementia: Diagnosis, Assessment & Disease Monitoring, 11(1), 450–462. https://doi.org/10.1016/j.dadm.2019.04.009



